Keratoconus & Pellucid Marginal Degeneration
Our Doctors Focus On Keratoconus Treatment
Dr. Steinhäuser is especially passionate about caring for patients with keratoconus and has special expertise in fitting advanced scleral lenses for keratoconus. The remainder of this section provides a concise overview of the condtion and its treatment. Feel free to contact us if you require information beyond what you find here or in the Keratoconus Links offered at the bottom of this page.
What is Keratoconus?
Keratoconus is a disorder that causes progressive thinning and distortion of the cornea - the clear dome at the front of the eye. The cornea normally has a rounded shape, but in keratoconus the thinned area bulges forward to produce a cone like protrusion. This results in progressive distortion and reduced vision. Many keratoconus patients experience blurred distance vision, glare, light sensitivity, disturbed night vision, headaches and reading problems. Keratoconus may affect only one eye but more commonly occurs in both eyes. It affects people of all races and both sexes. Most patients develop keratoconus in their late teens to early twenties, although it can begin at any age. Pellucid marginal degeneration (PMD) is a corneal thinning disorder related to keratoconus that primarily affects the inferior cornea.
Establishing the Diagnosis
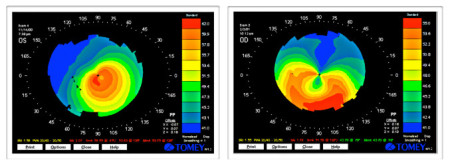
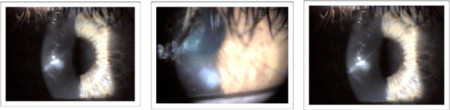
Patients who develop keratoconus often experience reduced vision as a first symptom. Nearsightedness and astigmatism (irregular curvature of the eye) are often the first signs of the disorder. Frequent prescription changes are another common sign of keratoconus. Before computerized corneal topography became available, it was sometimes difficult to establish a diagnosis of keratoconus, especially if the practitioner was not familiar with the early-stage symptoms of the disease. The classic signs of keratoconus include: Fleischer's ring (an iron colored ring surrounding the cone), Vogt's striae (stress lines caused by corneal thinning) and apical scarring (scarring at the apex of the cone).
Computerized corneal topography has facilitated the diagnosis of keratoconus, helping establish a definitive diagnosis earlier, follow progression more accurately and differentiate keratoconus from other conditions.
What Causes Keratoconus?
No one really knows what causes keratoconus. We do know that keratoconus runs in families and that many patients who have keratoconus report vigorous eye rubbing. Many patients with keratoconus also have allergies, but the link to allergic disease also remains unclear. Two theories for keratoconus have been proposed:
✓ Keratoconus corneas are more easily damaged by minor trauma such as eye rubbing.
✓ Keratoconus corneas lack the ability to self-repair routine damage easily repaired in normal corneas.
Although contact lenses have been suggested as a possible cause of keratoconus, this has not been proven and remains questionable. We advise patients with keratoconus to avoid eye rubbing as much as possible. Cold compresses applied to the eyes are helpful. Newer anti-allergy medications such as Pazep® or Zaditor® are also useful in managing itch and eye rubbing.
Treatment Options
We are great believers in conservative treatment. In the mildest form of keratoconus, eyeglasses or soft contact lenses often provide adequate vision.
In more advanced keratoconus, rigid gas permeable corneal or scleral contact lenses are usually the best choice for visual rehabilitation. There are numerous contact lens designs used to treat keratoconus and pellucid marginal degeneration. The Rose-K is an example of an exceptional and flexible corneal lens design originally introduced by New Zealand Optometrist, Dr. Paul Rose. Some of the newest ZenLens scleral lenses fitted using ultraprecise optical coherence tomography can provide exceptional comfort and outstanding vision for keratoconus patients. Scleral lenses have rapidly become a preferred choice for many patients.
The key to a successful contact lens fitting isn't as much the lens as it is the skill and experience of the contact lens fitter. Fitting contact lenses on a keratoconic cornea is delicate and time-consuming. You can expect several return visits to fine-tune the fit and prescription. In rare cases the process can take many months. For some patients it is a continuing process which begins all over again as the condition progresses. We do our best to keep it simple, but our primary focus will always be on you vision and the health of your eyes.
Fitting patients with PMD can be especially challenging. In the early stages, the central cornea is regular although highly astigmatic. Custom soft toric contact lenses will often provide adequate performance and safety. As the condition advances, specialized rigid and scleral lens designs provide viable options.
Improperly fit contact lenses can cause extensive damage to the cornea and can ultimately lead to a corneal transplant. Contact lens fitters should be selected on the basis of experience and commitment to aiding keratoconus patients. Having an advanced corneal topographer and several keratoconus contact lens trial sets available in the office are a positive sign.
If your cornea can't tolerate a contact lens, or contact lenses no longer provide acceptable vision, the next step is surgery ranging from corneal collagen crosslinking using riboflavin to INTACS® ring segment inserts or a traditional corneal transplant, also called a penetrating keratoplasty. We work closely with several leading corneal surgeons if the need arises.